Brookings Health Encourages Self-Testing for COVID-19
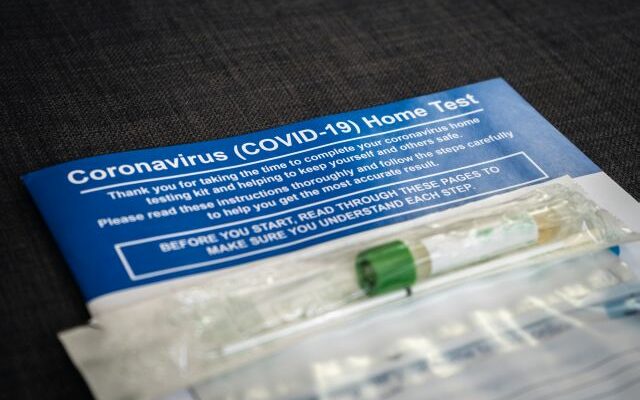
With the current rise in COVID-19 cases spread by the omicron variant, Brookings Health System encourages community members who have started experiencing mild COVID-19 symptoms or have been exposed to someone confirmed to have COVID-19 to use an at-home, self-test for diagnosis.
“We’re at a point in the pandemic where we need our community to wisely use clinic, urgent care and emergency room resources,” said Emergency Department Director Karen Weber. “If you’re not high risk, are experiencing mild symptoms or no symptoms at all, an at-home test can give you accurate results.”
Self-tests are available for purchase at local pharmacies and retailers. In addition, people may order free test kits from the South Dakota Department of Health at doh.sd.gov/COVID/Testing and the U.S. Federal Government at COVIDtests.gov. Also, the South Dakota Department of Health has begun distribution of 1-million free, at-home tests. Over the next few weeks they should become available at a number of locations including pharmacies.
COVID-19 self-tests are very reliable at detecting COVID when symptoms are present. If an at-home test is negative when symptoms are present, the cause is most likely another illness such as a cold or influenza.
If you test positive with a self-test, you do not need to retest elsewhere. Stay at home, inform your primary care provider and any close contacts, perform self-care and isolate. Current CDC guidelines state you should isolate for five days after you first experienced symptoms or had a positive viral test. If after day five you have no symptoms or fever, you can leave your house, but continue to wear a mask and avoid being around high-risk people for another five days.
Brookings Health encourages community members who are mildly to moderately sick with COVID-19 to follow supportive self-care and at-home treatment. Those measures include:
Get plenty of rest. Your body needs the energy to fight the illness. Do not take on big activities while staying at home; they can wait. COVID can get worse at the end of its course; it’s not unusual for days eight to 10 to be the hardest.
Stay hydrated. Try to drink six to eight glasses of liquids (water, sports drink, juice) per day, especially with a fever. Urine should look closer to lemonade than apple juice. If it is darker, drink more liquids. Avoid caffeinated beverages or alcohol.
Take over-the-counter (OTC) medications. Use acetaminophen/Tylenol or ibuprofen to reduce fever and pain. Keeping the fever down helps prevent dehydration and helps so the body doesn’t have to fight as hard. Use cough suppressants, nasal decongestants and chest expectorants as needed.
Prone. Cycle through the prone positions to help with your breathing and keep your lungs open. Change positions every 30 minutes to two hours in this order: 1) lying on your belly; 2) lying on your right side; 3) sitting up; 4) lying on your left side; 5) back to lying on your belly and repeat.
Take big, deep breaths. Taking two to three deep breaths every hour help gets oxygen deep in the lungs, assisting in clearing out mucous and other fluids.
Monitor oxygen levels. If you have an at-home pulse oximeter, monitor your oxygen levels to be sure they are over 90%.
Seek care if symptoms worsen. Seek medical attention immediately if you experience any of the following:
Difficulty breathing or increased shortness of breath. Persistent chest pain. Unable to keep fluids down. Unable to reduce fever with OTC medications. Increased weakness or falling. Inability to stay awake or new confusion. Bluish lips or face
“If you’re unable to manage your symptoms at home, call your primary care provider. If you experience very severe symptoms, we want to see you in the ER,” said Weber. “But please always call before you come to any provider so they can prepare for your visit and protect themselves from getting sick.”
More information about COVID-19 can be found online at brookingshealth.org/COVID.
January 24, 2022



